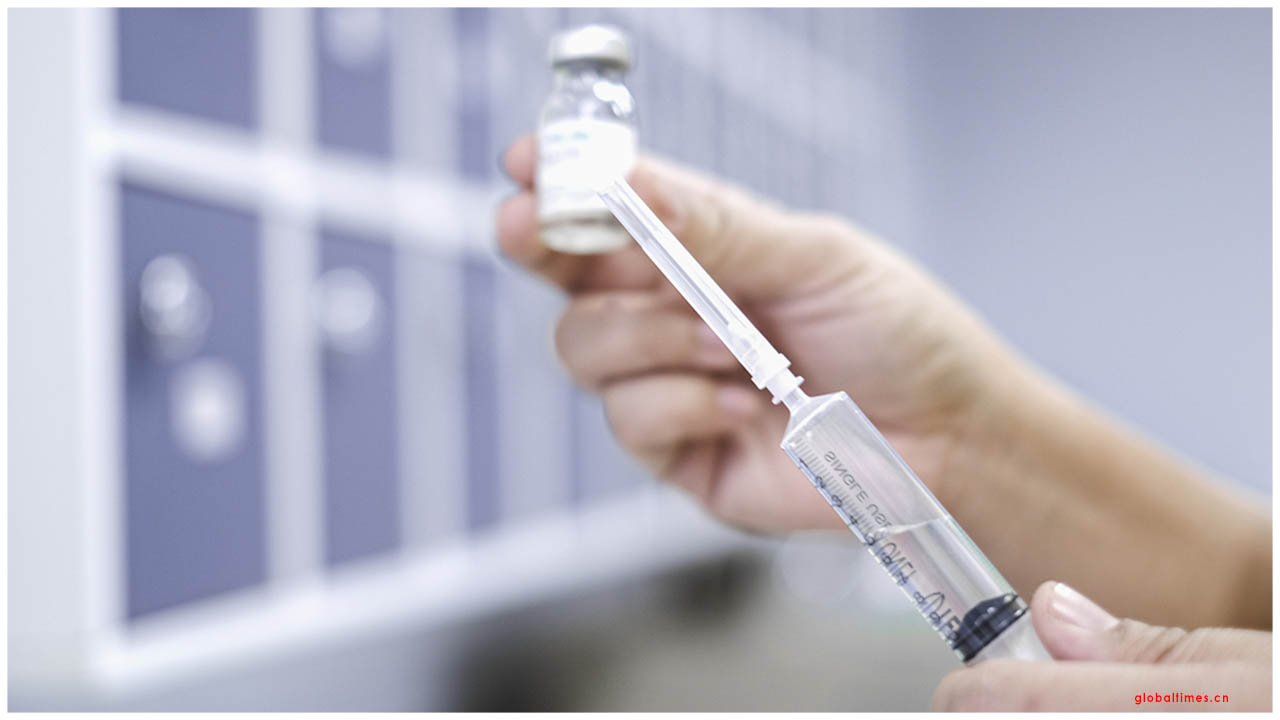
In late January 2020, the isolation ward at Souillac Hospital in the south of Port Louis had six people in quarantine. They had flown to the Mauritian capital from Wuhan city. This was long before the Indian Ocean island confirmed its first COVID-19 cases, but strict measures were already in effect to detect and prevent the virus from spreading.
When the country reported the initial cases on 18 March, it took just five weeks to bring down the infections from a cluster of local cases to zero cases, becoming the first in Africa to contain the spread of COVID-19. The achievement is largely credited to quick action in enforcing a raft of stringent preventive and control measures.
“Our national response was timely and decisive,” Prime Minister Pravind Kumar Jugnauth in August told the annual World Health Organization (WHO) Regional Committee meeting which gathers African health ministers and government representatives.
Soon after the first cases were detected, Mauritius imposed a nationwide lockdown, stepped up screening, contact tracing, and public awareness on preventive measures. It also enhanced testing and invested more resources in the response, procuring medicines, and equipment.
Rapid response teams were set up and posted at each regional hospital, and all health workers involved in COVID-19 prevention and control were equipped with personal protective equipment. The government also ensured the wellbeing of health personnel. All those working in quarantine or treatment centers were given 10 days off after each week of work, they would then be tested twice, and allowed to resume work if both tests were negative.
Health Minister Dr. Kailash Kumar Jagatpal said meticulous contact tracing “helped the country to saves many lives.” The national task force on COVID-19, which met daily and chaired by Prime Minister Jugnauth, made contact tracing, testing, and treatment the cornerstones of the response.
As of 31 August, Mauritius had done over 226 000 tests comprising 160 315 rapid antigens and more than 66 000 polymerase chain reaction tests – the COVID-19 gold standard diagnosis. It has only 11 active cases – all imported – and has had no local transmission since 26 April 2020.
The island nation’s experiences in managing malaria, chikungunya, and dengue outbreaks and its well-established surveillance system was a boon to COVID-19 detection and response.
Mauritius was among 13 African countries identified by WHO at the onset of the COVID-19 pandemic as being at high risk due to the high volume of international travel, high prevalence of non-communicable diseases, high population density, and long life expectancy – older people are considered to be at a greater risk of severe illness from COVID-19. Initial modeling by WHO predicted about 90 000 moderate, severe or critical cases and over 800 deaths in Mauritius if containment measures failed.
Thanks to the robust response the country has to date registered 356 cases and 10 deaths.
Huge political commitment, strong preparedness, and response coordination, in which WHO played a key role, has been instrumental in curbing the virus. “I appreciate that all the technical guidance is given by WHO has been taken on board by the Government of Mauritius,” said Dr. Laurent Musango, WHO Representative in Mauritius.
Much credit is also due to the country’s advanced public health system. Mauritius spends about 5% of its GDP on health. The sub-Saharan Africa average is around 6.2%. Mauritius scores as well as high-income countries in many health indicators such as life expectancy, infant or maternal mortality rates.
“To achieve universal health coverage, we have put in place a public health system which is free, accessible and sophisticated from primary health care to specialized services,” Prime Minister Jugnauth said, explaining that the country will invest some US$ 1.7 billion in the public health sector during the next five years.
“It is crucial to have an efficient health system at a time when we are experiencing the COVID-19 pandemic,” he said. “The government continues to invest significantly in the health sector for both present and future generations.”

 A WHO report on efforts by Mauritius to curbs COVID-19
A WHO report on efforts by Mauritius to curbs COVID-19